Preparing for Benedict’s Law: A Gap Analysis for Schools

Allergies are no trivial subject. With around two children in every classroom having a food allergy and approximately 30% of severe reactions occurring in children with no prior diagnosis, it is a growing and life-critical risk affecting children across all phases of education.
The discussion around Benedict’s Law and allergies is one about consistency, preparedness, and prevention, to ensure no child is put at unnecessary risk while in education.
What is Benedict’s Law?
Following numerous serious incidents and increasing concern on the inconsistency around how allergies are being dealt with, Benedict’s Law was introduced to set clear statutory expectations for how schools manage allergies safely.
This new guidance will replace previous non-statutory advice on supporting children and young people with medical conditions and allergies. At the moment, these protections are agreed to come into force in England in September 2026, but campaigning continues to extend it to Wales, Scotland, and Northern Ireland.
Understanding the New Statutory Requirements
With Benedict’s Law coming into full effect soon, schools in England must implement the following by September 2026:
- A Comprehensive Allergy Policy: Policies should cover prevention, response, and responsibilities, and must be regularly reviewed and communicated. These policies must be able to demonstrate how allergies are identified and managed, how risks are reduced across the school day, and how emergency situations are handled.
- Spare Adrenaline Auto-Injectors (AAIs): Schools will be required to hold spare AAIs and have clear procedure for their safe storage, checking, and emergency use.
- Whole-staff Allergy Awareness Training: All staff will have to understand allergy risks, symptoms of anaphylaxis, and emergency response. Best practice would be a mixture of online training with face-to-face learning for key identified personnel.
- Incident Reporting: A robust reporting system for allergy incidents and near misses is required, with further learnings integrated into Individual Healthcare Plans.
- Individual Healthcare Plans (IHPs): Pupils must have IHPs, which includes allergy triggers, day-to-day management, and emergency action steps.
- Inspection and Accountability: Ofsted will consider how well schools implement their allergy policies as part of inspections, meaning allergy safety is now a part of the safeguarding and leadership judgements.
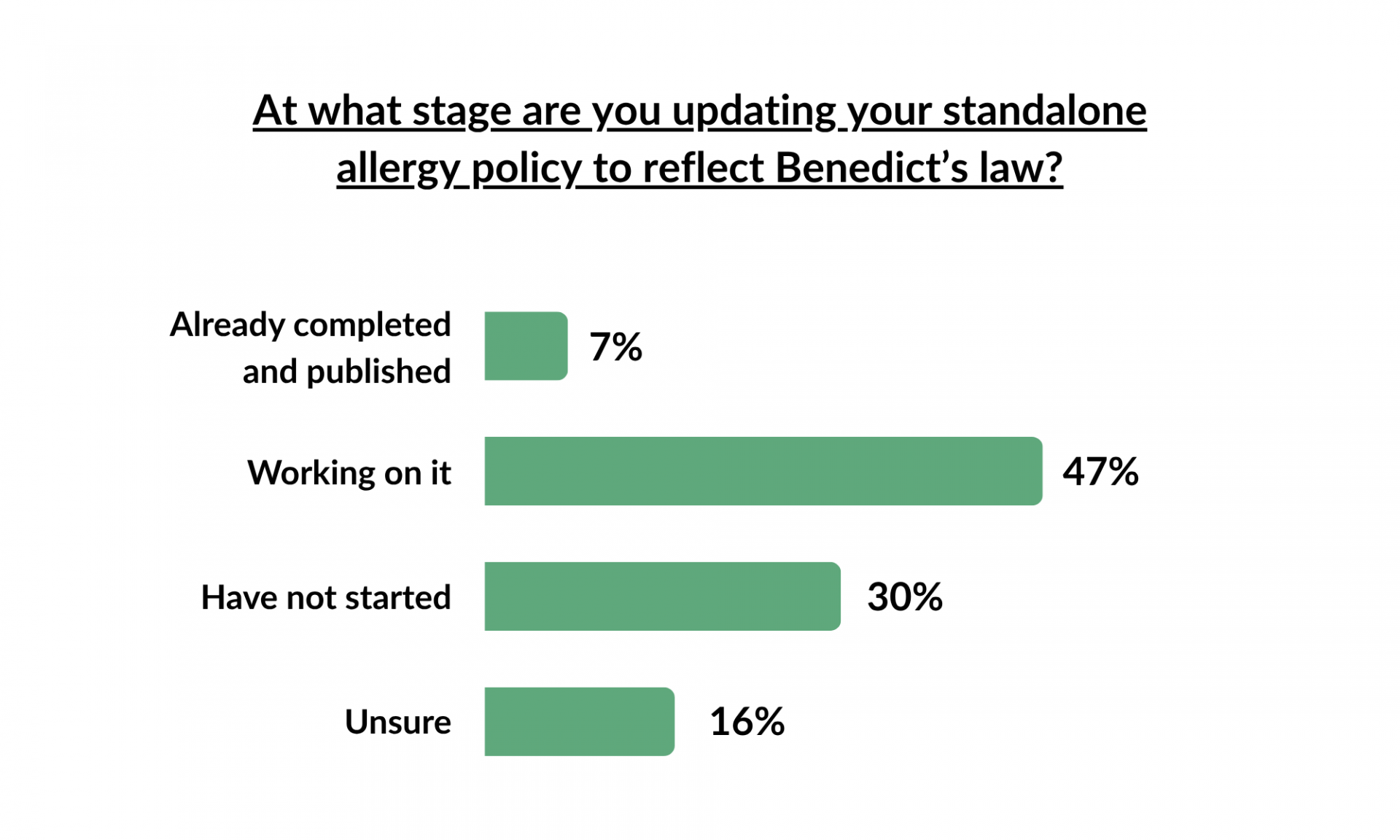
Gap Analysis & Readiness Planning
.png)
With the majority of our sofa session attendees mentioning that they are in the middle of updating their allergy policies or have yet to begin the process, there is no better time than now to conduct a gap analysis and look into readiness planning. The question to ask here is not whether you are compliant, but whether your system can still protect a child on days that are busy, disrupted, and short-staffed.
The Gap Analysis Framework
A non-exhaustive list of key considerations to stress test your current operations.
Strategic & Leadership Considerations
- Is allergy safety clearly recognised as a health & safety risk, not just a medical issue?
- Is there clear senior leadership ownership and accountability?
- Do governors or trustees have visibility and assurance?
- Are expectations consistent across the school or trust?
Identification & Information Flow
- Are allergies reliably identified at admission, transition, and change points?
- Is critical information easy to find quickly, especially for supply or temporary staff?
- Are updates communicated promptly and consistently?
- Does information flow across systems (MIS, risk assessments, care plans)?
Training & Competence
- Do all staff groups receive appropriate allergy training?
- Is training role specific, not generic?
- Is confidence tested through discussion or scenarios, not assumed?
- Is training refreshed regularly and built into induction?
Medicines & Emergency Response
- Is emergency medication immediately accessible without delay?
- Would access still be possible during evacuation, lockdown, or disruption?
- Is it clear who leads and who acts during an allergic emergency?
- Are allergic reactions embedded into emergency response planning?
Communication
- Are expectations with parents and pupils clear and consistent?
- Do contractors (catering, clubs, lettings) understand allergen controls?
- Is messaging consistent across the school or trust?
- Are responsibilities explicit, not implied?
Culture & Confidence
- Do staff see allergy safety as everyone’s responsibility?
- Are concerns raised early and taken seriously?
- Are near misses discussed and learned from?
- Is decision making supported, not second guessed?
Turning Gaps into Readiness
Once the gaps are identified, the goal would be to plan for readiness while incorporating a routine of review and learning. Readiness is not static; it requires a cycle of constant review and feedback. Successful planning focuses on two drivers:
- Prioritise Risk, Not Volume: Focus on high-severity and high-likelihood, sequence actions realistically, and understand that not everything can be addressed at once.
- Assigning Clear Ownership: While allergy safety is everyone’s responsibility, explicit ownership is needed, alongside a realistic timescale and a review mechanism. Having real ownership (a named role) help drive accountability and follow-through.
The Final Readiness Test
A well-conducted analysis should leave leadership able to answer one question honestly: “Would our systems protect a pupil if today was busy, disrupted, and short-staffed?”
If the answer is Yes: Your readiness planning is working.
If the answer is Maybe: Your gaps are now visible and must be prioritised.
If the answer is No: The gap analysis has done its job, it has identified a critical risk before an incident occurs.
Facilities & Food Safety Responsibilities
Facilities and catering teams play a critical role in allergy safety, including managing allergens in the kitchen, ensuring compliance with Natasha’s Law, robust special diet procedures, and clear labelling, segregation, and cleaning regimes.
Notably, allergy management is now a core component of unannounced Environmental Health inspections, directly impacting hygiene ratings and enforcement outcomes.
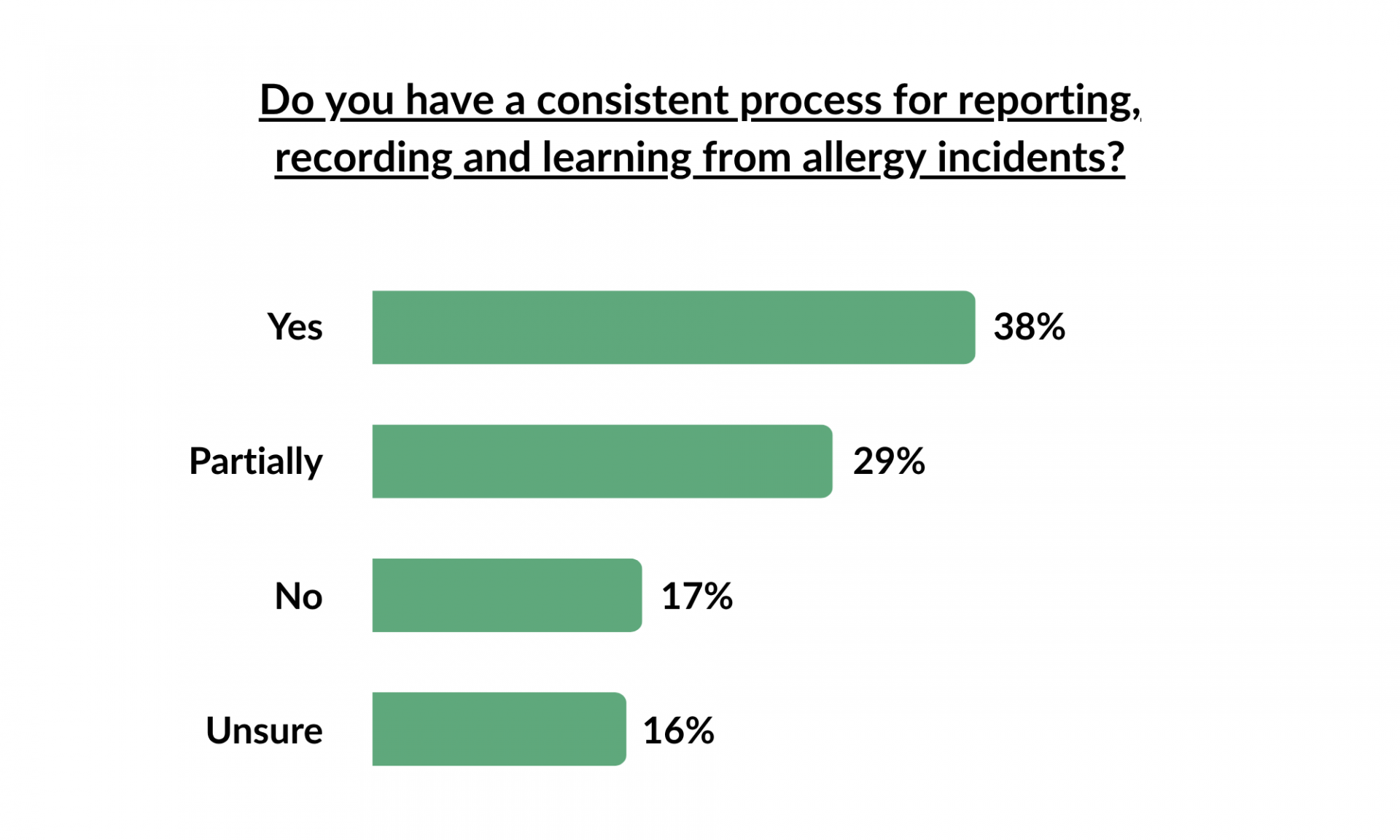
Your allergen policy should be a working document that is a true reflection of what happens at your school. This should include how pupil’s allergy information is obtained and how they are communicated to relevant parties, how pupils are identified at the point of service, as well as potential critical points where process may break down and actions in place to mitigate these risks.
Best practice would be to use a physical method of identification, such as a lanyard, card or badge, or in the case of senior schools the use of till systems to identify allergens for a specific pupil at the point of payment. It is also important to regularly review your processes with all stakeholders to ensure they match your allergen policy and the systems in place remain robust.
Health & Safety Integration
Allergy management should never sit in isolation.
Under Benedict’s Law, allergies are not simply a healthcare consideration, they are a foreseeable risk that must be controlled through existing health & safety systems. When allergy risk is treated separately, it becomes fragile, inconsistent, and overly dependent on individuals.
Risk Assessments
Allergy risk should be visible across all relevant risk assessments, not just IHPs, which includes:
- Classroom and curriculum activities (food use, science experiments, sensory play)
- Educational visits and trips (travel, catering, accommodation, emergency access)
- Events and celebrations (reward food, bake sales, festivals, PTA activities)
- Contractor and third-party activities (caterers, relief staff, after school providers)
Identify allergens as hazards with proportionate, realistic control measures. These controls should be proportionate and realistic, while being able to answer the question of what could go wrong if assumptions fail. Generic statements with no environmental or procedural detail or signposts like “refer to healthcare plan” should be avoided.
Managing Medicines and Treatment as a Safety-Critical Process
Emergency medication like Adrenaline Auto-Injectors (AAIs) should be treated with the same rigour as fire safety equipment. Rather than viewing them as "clinical items," schools must integrate them into core Health & Safety protocols. This means policies must explicitly recognise allergic reactions as immediate, life-threatening risks, ensuring medication is never locked away and remains accessible during evacuations, lockdowns, or staff absences. Effective systems anticipate human error and reduce dependence on individual memory.
Proactive Prevention Systems
While compliance focuses on meeting requirements, true prevention focuses on reducing the likelihood of harm before it occurs. Transitioning to a preventative culture requires three core systems:
Consistent Staff Training
Prevention relies on shared understanding, not isolated expertise. Training must be consistent across the Trust to avoid local interpretation risks and must include temporary or agency staff. The goal is ensuring every adult understands why allergy management matters, ensuring knowledge is refreshed rather than assumed permanent. 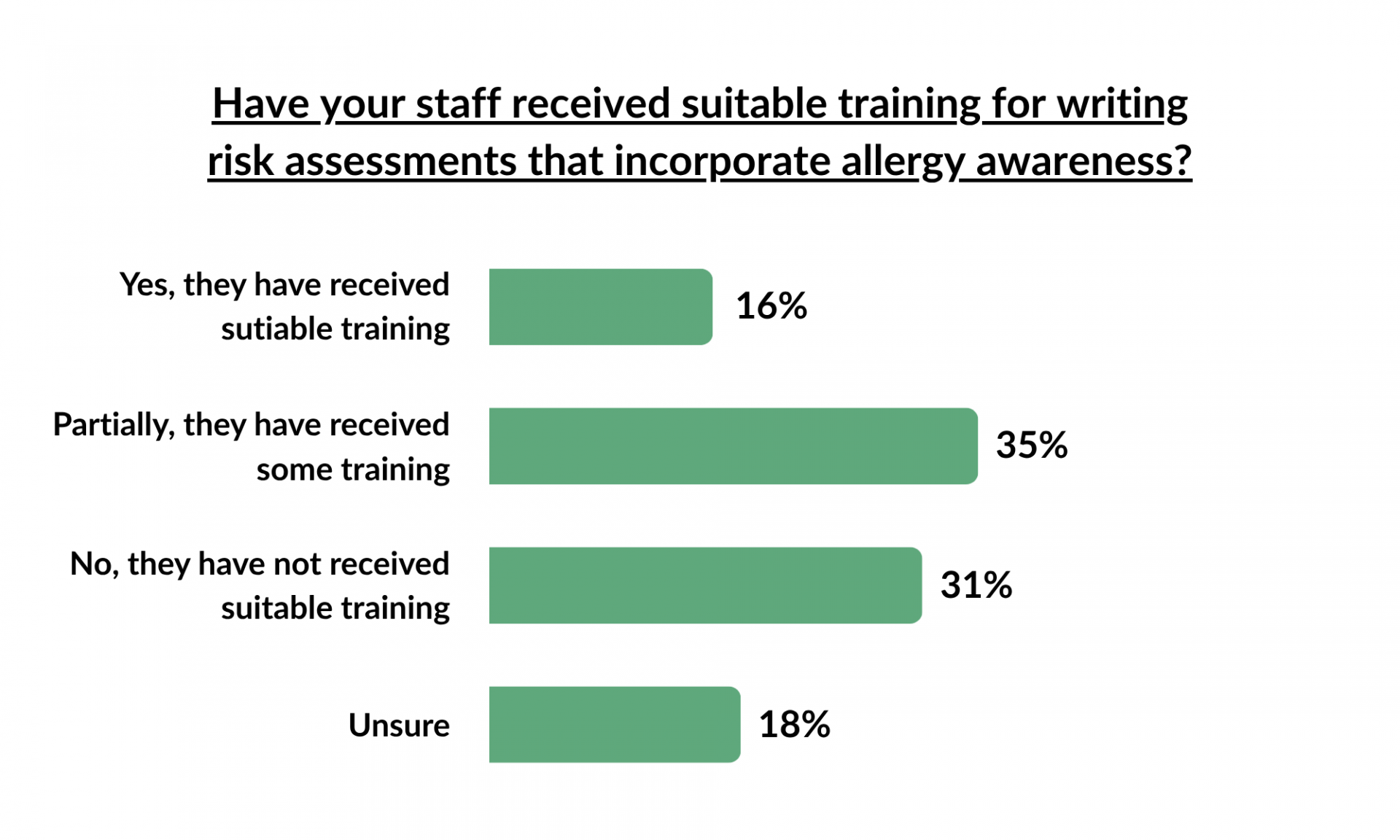
Predictable Communication
Effective systems remove assumptions. Schools must establish structured, two-way dialogue with parents and clear boundaries for contractors and third parties. Proactive leadership asks: "Are we relying on parents to fill our system gaps?" or "Could mixed messages undermine our controls?"
Reliable Identification and Flagging
Risk must be visible early. Data should be captured at every transition point and must flow with the pupil, not just the paperwork. By standardising recording across the Trust and integrating allergy data with safeguarding and SEN processes, schools ensure that essential information is accessible to staff exactly when they need it.
Do You Need a Hand?
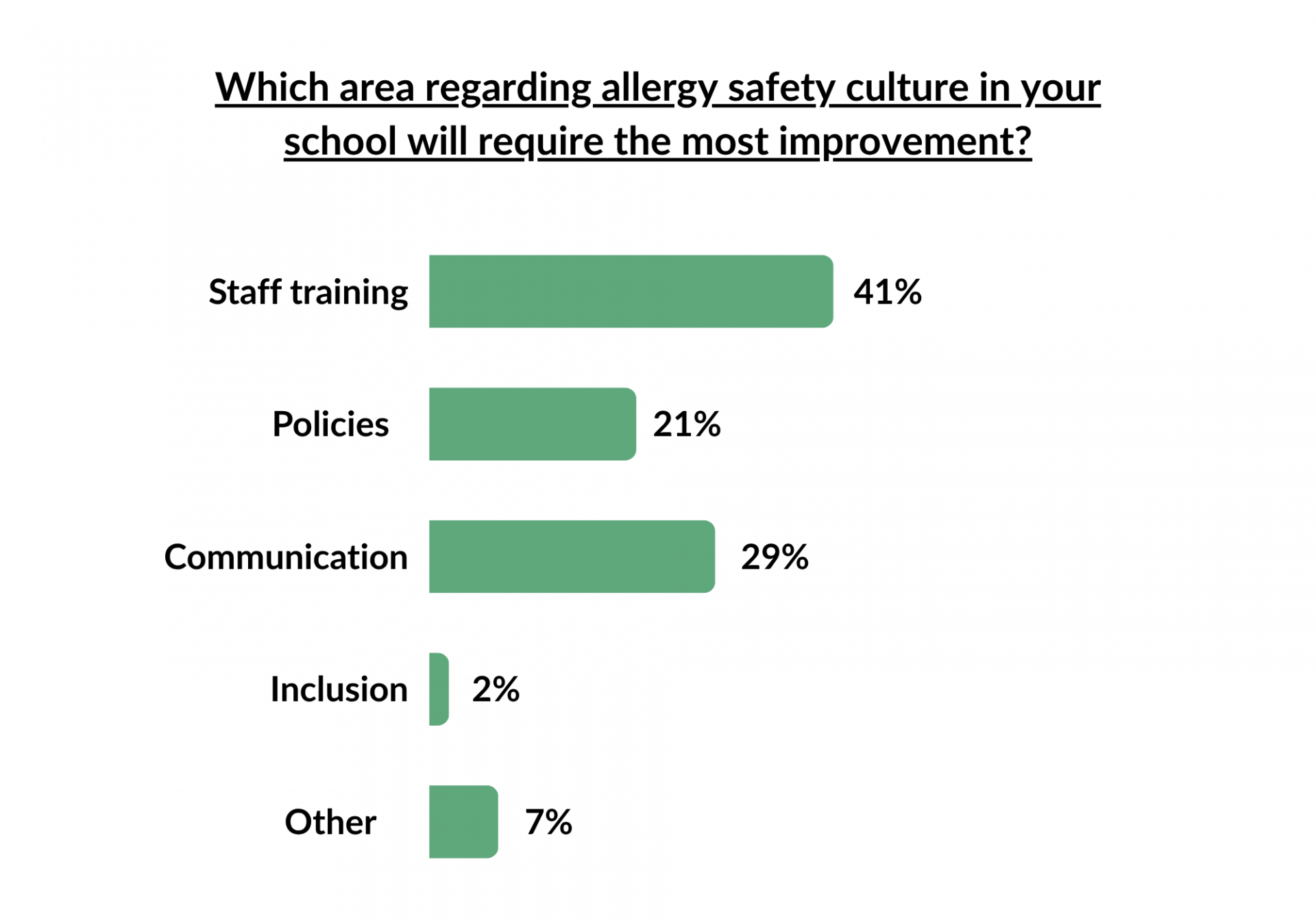
Benedict’s Law isn’t just a checklist, it’s a commitment. With Benedict's Law moving to a statutory requirement, there is widespread concern regarding the various areas of improvement schools must address to reach full readiness. This is exactly where Judicium Education can offer you peace of mind. Our Health and Safety Service is designed to support schools and trusts to embed practical, consistent safety systems that protect pupils and support staff confidence.
To support your readiness planning, our audit process is being updated to reflect Benedict's Law requirements in advance of the deadline, alongside relevant policies and templates on our Jedu platform. Furthermore, our Health & Safety clients will also have access to training courses on our eLearning platform to help ensure your entire staff is prepared ahead of time.
For more information regarding our Health and Safety Service, you can check our service page here.
If you would like to talk to someone about some support for your school or trust, do not hesitate to call us on 0345 548 7000 or email enquiries@judicium.com.
Follow us on X: @JudiciumEDU.
© This content is the exclusive property of Judicium Education. The works are intended to provide an overview of the sofa session you attend and/or to be a learning aid to assist you and your school. However, any redistribution or reproduction of part or all of the contents in any form is prohibited. You may not, except with our express written permission, distribute or exploit the content. Failure to follow this guidance may result in Judicium either preventing you from accessing our sessions and/or follow-up content.
Related content
(8).png)
Learn how the Martyn's Law impacts your school. From staff awareness to site-specific drills, discover how to meet Standard Tier requirements through proportionate, practical steps that build on your existing safety procedures.
.png)
This blog discusses new statutory guidance coming into effect in September 2026, with compulsory updates for schools across England regarding supporting pupils with allergies.
.png)
This blog is based on Judicium’s Health and Safety ‘Sofa Session’ from the 4th March 2026, with our resident expert Isthar Pearce. In this blog, we explore the importance of controlling risk when it comes to contractor safety and not just relying on paperwork, and provide actionable next steps for good practice.
.png)
This blog is based on Judicium’s Health and Safety ‘Sofa Session’ from the 7th January 2026, with our resident expert Jamie Ashard CMIOSH. This session focused on Common key stressors in the education sector, Applying the 6 key HSE management standards for stress, Completing a stress risk assessment and implementing practical solutions.
.png)
This blog is based on Judicium’s Health & Safety and SEND session on 26th November with resident expert India Cottenden
.png)
This blog is based on Judicium’s Food Safety Sofa session on 12th November with resident experts Sue Roberts and Tracey Killick

Sofa Sessions | H&S